Welcome to the New Dental Details!
MCNA is proud to present to you the first edition of the new Dental Details! We listened to your feedback about our monthly provider newsletter and identified your unmet communications and informational needs. In response, we have completely redesigned the look of your provider newsletter as well as the types of content included. Please take some time now to explore the new Dental Details. You will find news and updates about MCNA's programs and processes as well as information and tips useful in improving various aspects of your office operations. We hope you enjoy and we would love to hear your thoughts about it! Contact our Provider Hotline to let us know what you think.
MCNA Updates
MCNA is proud to present to you the first edition of the new Dental Details! We listened to your feedback about our monthly provider newsletter and identified your unmet communications and informational needs. In response, we have completely redesigned the look of your provider newsletter as well as the types of content included. Please take some time now to explore the new Dental Details. You will find news and updates about MCNA's programs and processes as well as information and tips useful in improving various aspects of your office operations. We hope you enjoy and we would love to hear your thoughts about it! Contact our Provider Hotline to let us know what you think. |
|
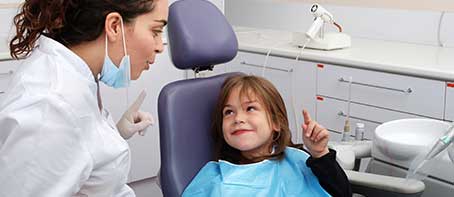
Clear Communication for Increased Health Literacy
Good communication is the basis for a successful dental visit. This is especially true when a member's oral condition requires a complex treatment plan. The more fully you can explain a diagnosis to a member and his or her parent, the more comfortable they will be with the treatment you propose. Communicating effectively during a dental appointment can help to increase the health literacy of both the member and the parent. Health literacy has been shown to be a factor in the successful utilization of oral and medical health services. Understanding an oral condition and the treatment it requires can positively influence compliance both during a dental visit and at home, when good oral hygiene habits must be practiced. Providing clear and easily understandable information about the member's oral condition helps to establish a strong trust relationship. The U.S. Department of Health and Human Services Office of Disease Prevention and ...
Communication
Good communication is the basis for a successful dental visit. This is especially true when a member's oral condition requires a complex treatment plan. The more fully you can explain a diagnosis to a member and his or her parent, the more comfortable they will be with the treatment you propose. Communicating effectively during a dental appointment can help to increase the health literacy of both the member and the parent. Health literacy has been shown to be a factor in the successful utilization of oral and medical health services. Understanding an oral condition and the treatment it requires can positively influence compliance both during a dental visit and at home, when good oral hygiene habits must be practiced. Providing clear and easily understandable information about the member's oral condition helps to establish a strong trust relationship. The U.S. Department of Health and Human Services Office of Disease Prevention and ... |
|

Clarification of Continuity of Care Requirements
In support of the rollout of the Managed Medical Assistance Program across the state, Florida Medicaid has issued regular "health care alerts" for providers to communicate important information and address critical issues. One of the key goals of the new program is to ensure that benefit recipients experience continuity of care. There should be no breaks in service coverage during the transition period, whether they are switching from one provider to another or to a different managed care plan entirely. Continuity of care is a priority for MCNA. We want to help all of our network providers fully understand the requirements of this process and recognize its importance to the health and well being of our members. We would like to encourage you to review the Florida Medicaid Health Care Alert about continuity of care and familiarize yourself with the timeframes, authorization requirements, and payment expectations contained within it. To go to the alert now, please click here.
Utilization Management
In support of the rollout of the Managed Medical Assistance Program across the state, Florida Medicaid has issued regular "health care alerts" for providers to communicate important information and address critical issues. One of the key goals of the new program is to ensure that benefit recipients experience continuity of care. There should be no breaks in service coverage during the transition period, whether they are switching from one provider to another or to a different managed care plan entirely. Continuity of care is a priority for MCNA. We want to help all of our network providers fully understand the requirements of this process and recognize its importance to the health and well being of our members. We would like to encourage you to review the Florida Medicaid Health Care Alert about continuity of care and familiarize yourself with the timeframes, authorization requirements, and payment expectations contained within it. To go to the alert now, please click here. |
|

Celebrating "Smilestones" with Kids
In recognition of National Tooth Fairy Day on August 22, consider sharing an "official" lost tooth certificate with parents to leave along with money when ...
Children's Corner
In recognition of National Tooth Fairy Day on August 22, consider sharing an "official" lost tooth certificate with parents to leave along with money when ... |

Outreach Toolkit: MCNA Oral Health Flyers
MCNA's Quality Improvement (QI) department operates a robust member outreach program in communities across the state. As part of this program ...
Quality Improvement
MCNA's Quality Improvement (QI) department operates a robust member outreach program in communities across the state. As part of this program ... |

Team Building: Making it Work
Good working relationships between the members of your office staff are integral to an efficient and positive office atmosphere. Sometimes, though, it is a challenge to unite individuals into a cohesive unit during the course of regular office activity. In such cases, team-building activities can be an excellent way to improve working relationships while having fun. These activities can range from highly structured games and exercises to more relaxed socialization. When planning to bring your team together for such activities, remember to be sensitive to their needs and personal preferences. Some individuals may have scheduling restrictions that may prevent them from participation outside of working hours. Others may have specific boundaries regarding things like physical contact and the sharing of personal information that should be taken into consideration. You do not want to plan any team building activity that will put a member of your staff into an uncomfortable position or that could lead to embarrassment. Team building activities can take many ...
Your Practice
Good working relationships between the members of your office staff are integral to an efficient and positive office atmosphere. Sometimes, though, it is a challenge to unite individuals into a cohesive unit during the course of regular office activity. In such cases, team-building activities can be an excellent way to improve working relationships while having fun. These activities can range from highly structured games and exercises to more relaxed socialization. When planning to bring your team together for such activities, remember to be sensitive to their needs and personal preferences. Some individuals may have scheduling restrictions that may prevent them from participation outside of working hours. Others may have specific boundaries regarding things like physical contact and the sharing of personal information that should be taken into consideration. You do not want to plan any team building activity that will put a member of your staff into an uncomfortable position or that could lead to embarrassment. Team building activities can take many ... |
|